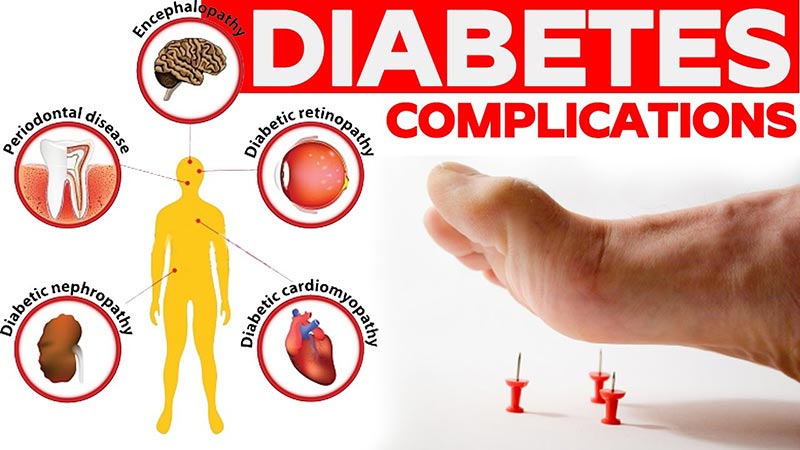
What are the Complications of Diabetes
Diabetes is dangerous not because it causes high blood glucose levels, but because it causes damage to any possible organ system. Diabetes is about broader upheavals in the body than many imagine, it is about disturbances in energy metabolism, fat metabolism, and changes in the anabolic processes. All this causes damage to blood vessels, nerves, and various organs. Diabetes is one of the leading cause of disabilities and mortality; it is the disease that causes complications leading to a shortened lifespan. Diabetes may not lead to many fatal outcomes directly, but indirectly, due to complications of diabetes, it affects lifespan.
Diabetic complications are often divided into two groups, acute and chronic. Acute are mostly result of undiagnosed, or uncontrolled, or poorly controlled diabetes, while chronic complications of diabetes are present in most living with diabetes. Chronic complications are difficult to prevent, but with adequate diabetes care their onset and progress may be delayed.
Acute complications of diabetes
Three common acute complications are Diabetic Ketoacidosis (DKA), Hyperglycemic Hyperosmolar States (HHS), and Hypoglycemia. All these complications are life-threatening, if not diagnosed promptly.
Hyperglycemic Hyperosmolar States (HHS)
It is uncommon and found in mostly undiagnosed cases of diabetes. In HHS blood sugar may go as high as 600 mg/dl or above (normal is 140 mg/dl after meals). High blood sugar starts a vicious cycle. The body tries to get rid of blood glucose by increasing urination, which further increases the glucose concentration due to dehydration. In HHS there would be significantly increased urination, thirst, fatigue, confusion. If not treated promptly, it may lead to coma and even death. A lab test would show unusually high glucose level (above 600 mg/dl), but without ketone bodies. HHS occur in people with severe insulin resistance and deficit, though they have enough insulin in blood to stop the formation of ketone bodies. Treatment would be in the hospital with IV fluids and insulin.
Diabetic Ketoacidosis (DKA)
Diabetic ketoacidosis is more common in type 1 diabetes, and occur due to poorly controlled diabetes, inadequate insulin level, missed insulin dosage, or suboptimal treatment. In insulin deficiency, there is high blood glucose. Nonetheless, body cells are starving as glucose is unable to enter the cells. Thus body tries to fulfill energy needs through an alternate pathway, by mobilizing fats, making ketones in the liver. Excess of ketones is harmful to health. Symptoms of DKA are nausea, vomiting, stomach pain, fruity odor, frequent urination, weakness, confusion, heavy breathing, and finally, it may cause coma. In DKA blood glucose is quite high, though not like HHS, and person tests positive for ketones. Treatment would be with IV fluids and insulin.
Hypoglycemia
Hypoglycemia is a complication of diabetes treatment and occurs in those on insulin therapy. It is rare with oral drugs. This is a condition when glucose falls below 70 mg/dl and brain does not get enough energy. Symptoms are shaking, rapid heartbeat, blurring of vision, behavior changes, seizures, and loss of consciousness. In most cases, it is treatable with sugary drinks or glucose.
Chronic complications of diabetes
Chronic complications of diabetes occur due to high blood glucose, dyslipidemia, insulin deficit, chronic inflammation, presence of AGEs (advanced glycation endproducts). These complications affect blood vessels, nerves, and working of organs. They are present in everyone living with diabetes, though diagnose of everybody is not happening. Vascular damage plays an essential role in the development of these complications leading to heart attack, stroke, kidney damage, amputations and so on. These complications are often divided into two big groups, microvascular (small blood vessels) complications, and macrovascular (large blood vessels) complications.
Microvascular Complications of Diabetes
- Diabetic retinopathy– one of the leading causes of preventable blindness. In this condition, damage of small blood vessels to retina happens, they often break down, causing small hemorrhages. Retinopathy depends both on the duration and severity of diabetes. There are involvement of various mechanisms, from the deficit of growth factors to metabolic changes. Deposition of fats also occurs at places of hemorrhages. In some cases, formation of new blood vessels (proliferative retinopathy) may only worsen the vision. Thus everyone with diabetes must have a regular ophthalmological checkup.
- Diabetic nephropathy– diabetes is the leading cause of damage to the kidney. More than one-third cases of renal failure are due to diabetes. In fact, 7-10% of those living with diabetes already have some signs of ensuing renal damage. Best prevention of renal damage is by adequate blood glucose control and blood pressure treatment. Newer antihypertensive drugs like ACE inhibitors and ARBs are also renoprotective.
- Neuropathy– is one of the most common complications with more than half of those with diabetes have neuropathy to some extent. Presentation of neuropathy varies considerably, in some people, one nerve may be damaged, while in other multiple nerves may be involved. In some, there may be alterations in sensory nerves (especially hand and feet), while in other motor neurons may be affected. Autonomic neuropathy is also common in diabetes, which results in the altered functioning of internal organs. There is no drug that may completely prevent neuropathy. However, strict blood glucose control may help. In severe painful neuropathy, doctors may prescribe antiseizure medicines, antidepressants, painkillers, along with supplements to improve nerve metabolism (alpha lipoic acid, vitamin B).
Macrovascular Complications of Diabetes
In diabetes there is endothelial dysfunction, meaning that internal walls of blood vessels are not healthy. Further, in diabetes, elevation of LDL and triglyceride levels occurs. Alteration of platelet aggregation is also happening. All this means that those living with diabetes are at higher risk of accumulation of fat in arterial walls, blockage of large blood vessels.
Numerous studies confirm higher risk of cardiovascular complications in diabetes. Those with diabetes are at higher risk of sudden heart attack or myocardial infarction. Most leading diabetes and heart associations agree that diabetes is a risk factor for heart diseases.
Blockage of large blood vessels is not just about heart attack, another life-threatening condition associated with it is stroke or blockage of blood vessels in the brain. Statistics indicate that diabetes increases the risk of stroke by 150-400%. Stroke can be fatal, or it may lead to disabilities.
Those at higher risk of vascular disease, with a family history of vascular conditions, need more aggressive treatment of diabetes. Thus there is a need for aggressive blood glucose management, need to control levels of bad cholesterol, and take drugs to reduce platelet aggregation (like low dose aspirin).
To prevent macro and microvascular complications of diabetes one must get a thorough medical checkup every 3 to 6 months. Control blood glucose levels, take medications regularly. Do not neglect lifestyle changes, like quitting smoking and doing regular exercise. Finally, one should also realize the importance of self-monitoring. Self-body-weight monitoring and control, self-blood-glucose tracking, self-blood-pressure monitoring, and so on.












UK Prospective Diabetes Study Group. Efficacy of atenolol and captopril in reducing risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 39. UK Prospective Diabetes Study Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38.